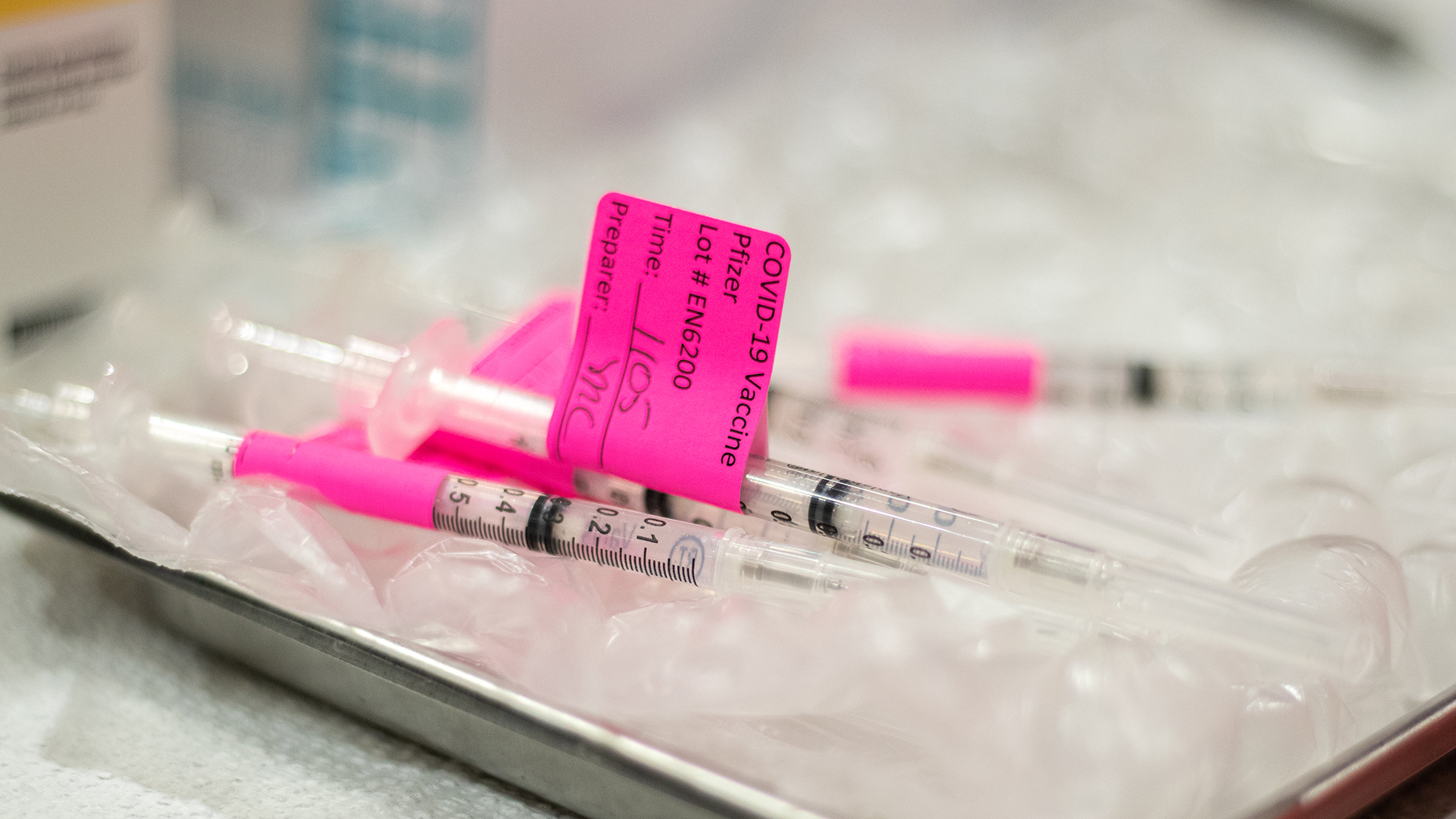
With three FDA-approved vaccines and state rollout underway, there is still hesitancy among communities of color, where history has shown that medicine won’t always be kind to them.
Following the launch of a campaign that supports COVID-19 vaccinations, University System of Maryland presidents highlighted the efficacy of the vaccine and the need to build trust in communities where vaccine hesitancy exists.
Statewide, only 68,329 Black or African American individuals have gotten their second doses.
In Prince George’s County, only 3.4 percent of the population has received their second vaccination dose. Black or African Americans make up the highest majority with 16,484 doses. But Hispanic and Asian vaccinations are lower — not even passing 2,000.
The university system released a campaign earlier this month voicing their support and confidence in the vaccine. It was an effort to garner trust in communities where people may be hesitant to take it.
University of Baltimore President Kurt Schmoke said the history behind this hesitancy could be described in one word: Tuskegee.
In 1932, 600 Black men in Macon County, Alabama entered a study that aimed to research syphilis under false pretenses. Of the 600 men, 339 had latent syphilis. The men were told they would be getting treated, but during the 40 years of the experiment, they never received real health care, even when penicillin became a viable treatment for syphilis 15 years later.
When the study was finally shut down in 1972, more than 100 participants had died of syphilis, and the disease had been spread to at least 40 spouses and 19 children at birth.
[USM university presidents promote COVID-19 vaccine in video presentation]
“The Tuskegee experiment is well-known throughout the country … and it simply was the most high-profile example of institutional medicine [treating] people of color with disrespect,” Schmoke said.
The Tuskegee study sowed tremendous mistrust within communities of color, particularly Black communities, but it wasn’t the only incident. Schmoke said that with John Hopkins University nearby and with the institution’s history of taking advantage of Black patients, Baltimore residents are even warier.
In 1951, white doctors at John Hopkins Hospital took cancerous cervical cells from Henrietta Lacks, a 31-year-old Black woman, without her consent or knowledge. Doctors passed along her cells to researchers who found her cells had an amazing capability to survive and reproduce. They shared it widely with other scientists, also without Lacks’ consent or knowledge. They became known as HeLa cells, which have been the base for most modern medicine today.
Like Tuskegee, the story of Henrietta Lacks brought to light ethical issues with medicine and highlighted the systemic racism within medical practice and research. Dealing with and knowing about that racism adds stress on an individual, said Dr. Mia Smith-Bynum, a professor in this university’s public health school.
And higher stress is just one factor in a myriad of social, economic and health issues that makes it so important for communities of color to get vaccinated, said Smith-Bynum.
For starters, many people of color are essential workers, she said. But she dived deeper with socioeconomic status and the social determinants of health, meaning the economic and social conditions that affect a group’s or individual’s health status.
Because of systemic racism, people of color tend to live in lower-income neighborhoods. They might live in food deserts, so there are fewer options for healthy nutrition. They have to work more and therefore have less time to exercise. There’s also higher amounts of stress that wear down the body.
All of these factors put these racially segregated communities at a higher risk for conditions such as diabetes, Smith-Bynum said. These communities have to deal with medical mistrust, stress and underlying health conditions that make them more susceptible to contracting the virus, she said.
“It’s like a trifecta of challenges here,” she said.
[A $1.4 billion proposal from Gov. Hogan could soften the pandemic’s blow to the USM budget]
Even though these communities are some of the ones that need to take the vaccine the most, the challenge lies in making them trust it first, Smith-Bynum said.
University of Maryland, Baltimore County President Freeman Hrabowski believes that’s why the university system’s campaign is so important. With the system being led by a diverse group of academic leaders, it adds credibility, he said.
But there’s more credibility in the fact that people of color as doctors and scientists are behind the vaccine as well, he said. Dr. Kizzmekia Corbett, a UMBC graduate, was at the forefront of developing the Moderna vaccine at the National Institutes of Health. Hrabowksi and his wife participated in the Moderna vaccine trials she led last August and September.
“When people say you don’t have trust, it’s from a time when scientists were white and the doctors were white and they were experimenting on Black people,” he said.
For Hrabowski, it’s extremely important for these communities to get vaccinated because it protects the individual but it also protects their family. If we want to see our friends and family, he said, we have to be safe.
Smith-Bynum agreed with Hrabowski’s sentiment of diversity within the medical world, but said that the campaign and representation alone won’t be enough to instill trust within Prince George’s County communities. It’s a great first step, she said, but there must be a more personal approach to get the message directly to these individuals.
Schmoke said the campaign started some of this personal dialogue between him and concerned members of his community. They had extensive conversations about policy issues, religious views and privacy rights.
Smith-Bynum went to her mother’s church recently to speak about the vaccine and said it was very well-received. But it can’t just be the people in community churches. It also has to be the directors of Boys and Girls Clubs and school principals speaking out in support of vaccination.
“It’s got to be the folks who already have relationships with the target population and the trust,” Smith-Bynum said.